Key Takeaways
- Bone loss begins immediately after tooth extraction — up to 63% of horizontal bone width can be lost within the first 6 months.
- Vertical bone loss averages 11–22% in the same period, with the fastest resorption occurring in the first 3 months.
- Socket preservation (bone grafting at the time of extraction) can reduce bone loss by up to 50% compared to unassisted healing.
- Delaying dental implant placement beyond 6 months significantly increases the likelihood of needing additional bone grafting — adding $1,500–$5,000+ in costs and months of healing time.
- 3D CT/CBCT imaging is essential for accurately assessing remaining bone volume before planning implants or grafting.
If you’ve recently had a tooth pulled — or you’re planning an extraction — there’s something your dentist may not have fully explained: bone loss after tooth extraction is not a possibility. It’s a certainty. The only question is how much bone you’ll lose and how fast it happens.
This matters enormously if you’re considering dental implants, because implants require a minimum amount of healthy bone to anchor into. The longer you wait after extraction, the less bone you have — and the more complex (and expensive) your implant treatment becomes.
Here’s what the research shows, what you can do about it, and why timing is the single most important factor in your treatment plan.

What Happens to Bone After Tooth Extraction?
Your jawbone exists for one reason: to support your teeth. Every time you chew, bite forces transmit through your tooth roots into the surrounding bone, sending signals that stimulate bone remodeling — the continuous cycle of old bone being broken down and new bone being formed. This mechanical stimulation is what keeps your jawbone dense and healthy.
When a tooth is removed, that stimulation disappears. The bone that surrounded the tooth root — called the alveolar bone — begins to resorb (break down) because the biological signals that maintained it are gone. This process is called alveolar ridge resorption, and it follows a predictable pattern:
- Inflammatory phase (days 1–7). The extraction socket fills with a blood clot. Inflammatory cells arrive to begin cleaning the wound. Osteoclasts (bone-dissolving cells) activate along the socket walls.
- Rapid resorption phase (weeks 1–12). The buccal plate — the thin wall of bone on the cheek side of the socket — resorbs fastest because it’s the thinnest. New woven bone begins filling the socket interior, but the outer walls are shrinking simultaneously.
- Remodeling phase (months 3–12). Socket fill continues, but the overall ridge dimensions continue decreasing. The rate of loss slows but doesn’t stop.
- Chronic atrophy (year 1+). Slow, ongoing resorption continues indefinitely at a reduced rate, gradually shrinking the ridge further over years and decades.
The Bone Loss Timeline: What Research Shows
The clinical data on post-extraction bone loss is extensive and consistent. Here are the key numbers from peer-reviewed research:
First 6 Months
A landmark systematic review by Tan et al. published in Clinical Oral Implants Research (2012) analyzed 20 clinical studies and found:
- Horizontal bone loss (width): 29–63% reduction, averaging 3.79 mm
- Vertical bone loss (height): 11–22% reduction, averaging 1.24 mm on the buccal side
A more recent meta-analysis by Agarwal et al. in the Journal of Prosthodontics (2019) confirmed similar findings, reporting a mean horizontal reduction of 3.87 mm and vertical reduction of 1.67 mm at 6 months post-extraction.
The Critical First 3 Months
Research by Araujo and Lindhe published in the Journal of Clinical Periodontology showed that approximately two-thirds of total ridge resorption occurs within the first 3 months. The buccal bone plate — which is often less than 1 mm thick — can resorb completely within 8 weeks in some patients.
First Year and Beyond
By 12 months, studies report total horizontal loss of 5–7 mm in many cases. After the first year, resorption slows to approximately 0.5–1% per year but never fully stops. Over decades, this chronic atrophy can leave patients with a dramatically reduced ridge that complicates implant placement, denture fitting, and even facial aesthetics.
| Timeframe | Horizontal Loss (Width) | Vertical Loss (Height) |
|---|---|---|
| 0 – 3 months | 2 – 4 mm (most rapid phase) | 0.5 – 1.5 mm |
| 3 – 6 months | 1 – 2 mm additional | 0.5 – 1 mm additional |
| 6 – 12 months | 0.5 – 1 mm additional | 0.2 – 0.5 mm additional |
| 1+ years | ~0.5 – 1% per year | ~0.5 – 1% per year |
| Total at 6 months | 29 – 63% of original width | 11 – 22% of original height |

How Much Bone Loss Is Normal?
All extraction sites experience some degree of bone resorption — it’s a universal biological response. The question is whether the amount of loss is within a range that still supports future treatment options.
As a general guideline, a standard dental implant requires a minimum of 6 mm of bone width and 10 mm of bone height at the placement site. If your post-extraction ridge has resorbed below these thresholds, bone grafting will be necessary before or during implant surgery.
What’s “normal” varies by location in the mouth:
- Front teeth (incisors): The buccal bone plate is extremely thin (often <1 mm). These sites experience the most dramatic visible resorption and often require socket preservation at the time of extraction.
- Premolars: Moderate resorption. The buccal plate is slightly thicker, but still susceptible to significant loss.
- Molars: The multi-rooted extraction site creates a larger socket. While more bone is lost in absolute terms, the surrounding bone tends to be thicker and more resilient, particularly in the lower jaw.
Factors That Accelerate Bone Loss
While every extraction leads to bone loss, certain factors make it significantly worse:
- Traumatic extraction. Extractions that require significant force, bone removal, or sectioning cause more damage to the surrounding bone and accelerate resorption. Research in the International Journal of Oral Surgery shows that atraumatic extraction techniques preserve up to 30% more bone.
- Infection at the time of extraction. Active periodontal disease or periapical abscess means bone loss has already begun before the tooth is removed. Post-extraction resorption compounds existing damage.
- Thin buccal bone plate. Patients with naturally thin buccal plates (common in the upper front teeth) lose proportionally more bone because there’s less to start with.
- Smoking. Tobacco use reduces blood flow to healing tissues and impairs bone regeneration. A 2018 study in Clinical Oral Investigations found that smokers experienced 23% more horizontal bone loss than non-smokers at 6 months post-extraction.
- Systemic conditions. Uncontrolled diabetes, osteoporosis, and certain medications (bisphosphonates, long-term corticosteroids) affect bone metabolism and healing.
- Multiple adjacent extractions. Removing several teeth in a row eliminates the inter-dental bone septae (the thin walls of bone between tooth sockets), resulting in more extensive ridge collapse.
- Wearing a removable denture. Conventional dentures press on the ridge, accelerating resorption through mechanical pressure on tissue not designed to bear load.
How to Prevent Bone Loss After Extraction
The most effective strategy is proactive intervention at the time of extraction — not after the damage is done. Here are the evidence-based approaches:
1. Socket Preservation (Ridge Preservation Grafting)
This is the gold standard. Immediately after extraction, the socket is filled with bone graft material and covered with a membrane. A 2015 Cochrane systematic review found that socket preservation reduces horizontal bone loss by 1.89 mm on average compared to unassisted healing — roughly a 50% reduction.
Types of graft materials used:
- Autograft: Your own bone, harvested from another site. Gold standard for biological compatibility.
- Allograft: Processed human donor bone. Most commonly used in socket preservation due to ease of handling.
- Xenograft: Bovine or porcine bone mineral. Excellent scaffold properties with slow resorption.
- Alloplast: Synthetic bone substitute (calcium phosphate, bioactive glass). Predictable and readily available.
2. Immediate Implant Placement
Placing a dental implant directly into the extraction socket — when conditions allow — is the most effective way to preserve bone. The implant immediately takes over the function of the tooth root, providing the mechanical stimulus that maintains bone volume. A 2020 meta-analysis in Clinical Implant Dentistry and Related Research showed that immediate placement preserved significantly more buccal bone than delayed placement protocols.
3. Platelet-Rich Fibrin (PRF)
PRF is a concentrated preparation of growth factors derived from your own blood. When placed in the extraction socket — alone or combined with bone graft — PRF accelerates soft tissue healing and provides growth factors that support early bone regeneration. While not a substitute for bone grafting, PRF is a valuable adjunct that improves healing quality.
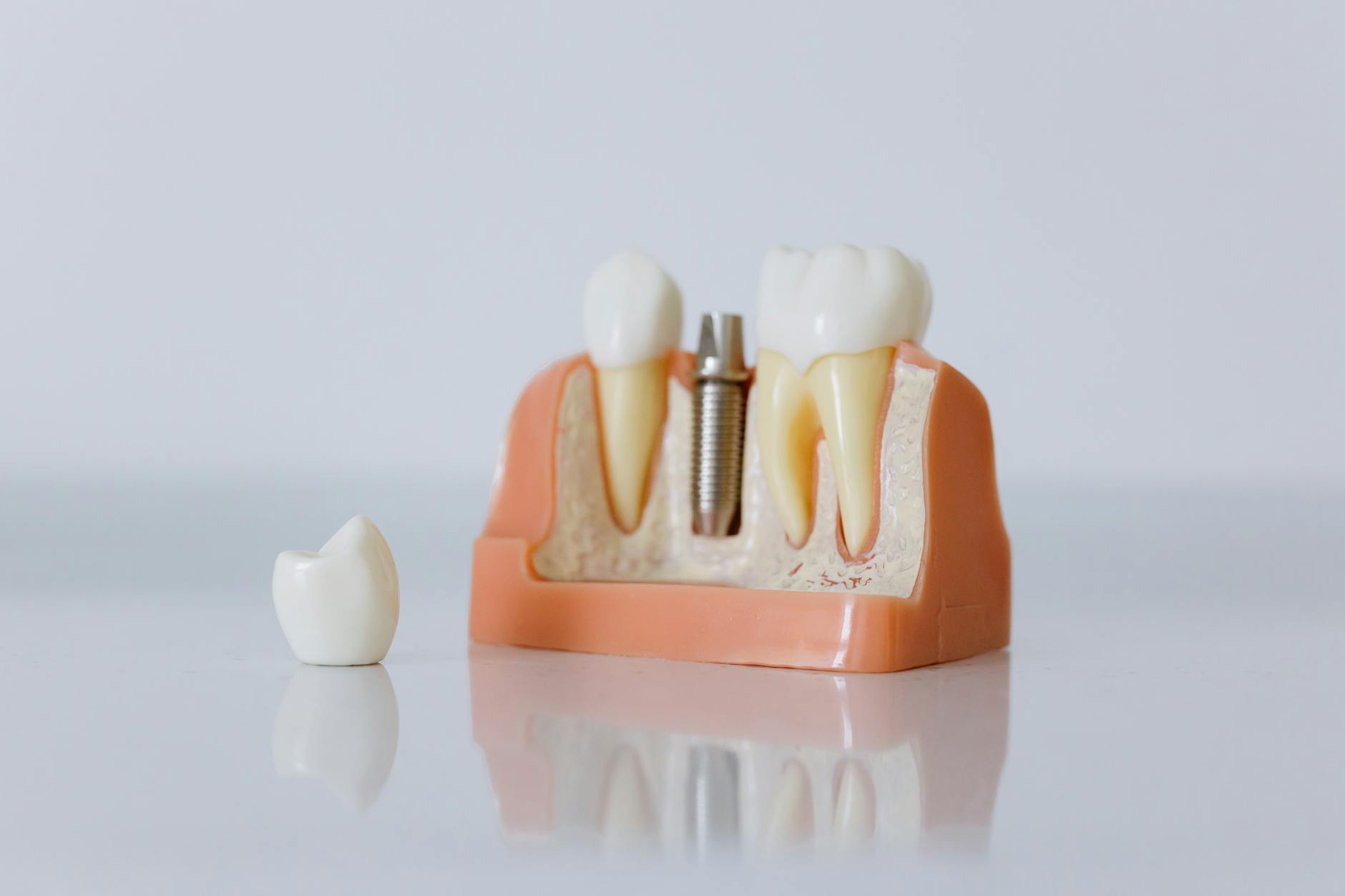
Bone Grafting: Your Best Defense
If the window for socket preservation has passed and significant bone loss has already occurred, bone grafting can rebuild the ridge to support dental implants. The approach depends on the extent of loss:
Minor to Moderate Bone Loss
Guided bone regeneration (GBR) uses bone graft material and a barrier membrane to rebuild bone in deficient areas. This is often done simultaneously with implant placement, adding no additional surgery. Healing time: 4–6 months.
Significant Vertical Loss
Block bone grafts or distraction osteogenesis may be needed. These are more complex procedures that require a separate surgery before implant placement. Healing time: 6–9 months before implants can be placed.
Severe Upper Jaw Loss
When the upper back jaw has lost significant bone and the maxillary sinus has expanded downward (pneumatization), a sinus lift procedure is needed. Bone graft material is placed beneath the sinus membrane to create adequate height for implants. Healing time: 6–9 months.
The cost of bone grafting adds $1,500–$5,000+ to your implant treatment, depending on the type and extent of grafting required. This is money that socket preservation at the time of extraction could have saved you.
Why Timing Matters for Dental Implants
This is the most important section of this article. The relationship between extraction timing and implant outcomes is well documented — and the data overwhelmingly supports acting early:
Immediate Placement (Same Day as Extraction)
When bone quality and quantity allow, placing an implant immediately into the extraction socket offers the best preservation of hard and soft tissue. Success rates for immediate implants are comparable to delayed placement — above 95% — when patient selection criteria are met. Not every case qualifies, but when it’s appropriate, it’s the ideal scenario.
Early Placement (4–8 Weeks Post-Extraction)
Allows initial soft tissue healing while the bone is still close to its original dimensions. Minimal additional bone loss has occurred. This is a common approach when the extraction site had infection that needed to resolve first.
Delayed Placement (3–6 Months Post-Extraction)
By this point, the rapid resorption phase has occurred. Many patients will need some degree of bone grafting to compensate for lost width. Still a very manageable timeline, but costs and complexity increase.
Late Placement (6+ Months Post-Extraction)
Significant bone resorption has occurred. The majority of patients at this stage require bone grafting, which adds 4–9 months of healing time before implants can be placed. What could have been a single-stage procedure becomes a multi-stage, multi-visit treatment plan with substantially higher costs.
The clinical message is clear: if you’re planning to replace an extracted tooth with an implant, discuss timing with your dentist before the extraction happens — not months later. At Smile Dental Center, we use 3D CT/CBCT imaging to evaluate your bone and plan the optimal approach, whether that’s immediate placement, socket preservation, or a staged protocol.
For patients who have already experienced significant bone loss and are exploring full-arch solutions, All-on-4 implants are specifically designed to work with reduced bone volume — often avoiding the need for extensive grafting entirely.
Frequently Asked Questions
Can bone loss from tooth extraction be reversed?
Yes, through bone grafting procedures. While you can’t naturally regrow bone that has resorbed, guided bone regeneration, block grafts, and sinus lifts can rebuild the ridge to a volume sufficient for dental implants. The success rate for bone grafting procedures exceeds 90% in published literature. However, it’s always preferable to prevent bone loss with socket preservation than to try to rebuild it later — prevention is faster, less invasive, and less expensive.
How long after extraction can I get a dental implant?
It depends on the clinical situation. Immediate placement (same day) is possible when bone quantity and quality are adequate and there’s no active infection. Early placement at 4–8 weeks is common when some initial healing is needed. If you’ve waited 6+ months, implants are still possible, but bone grafting may be required first, adding 4–9 months to the overall timeline. The bottom line: consult with your implant dentist before the extraction to plan the optimal timing.
Does bone loss after extraction cause facial changes?
Yes, particularly when multiple teeth are lost. As the alveolar ridge resorbs, the lower third of the face gradually collapses — the chin rotates forward, the lips lose support and appear thinner, and the nasolabial folds deepen. This is especially noticeable in patients who have worn removable dentures for many years. A study in the Journal of Prosthetic Dentistry (2018) documented measurable changes in facial profile as early as 12 months after multiple extractions without ridge preservation.
Is socket preservation worth the extra cost?
Almost always. Socket preservation typically costs $500–$1,500 at the time of extraction. If you skip it and need bone grafting later for implant placement, the grafting procedure costs $1,500–$5,000+ and adds 4–9 months of healing. Beyond the financial math, socket preservation also leads to a simpler, more predictable implant surgery with less post-operative discomfort. The International Journal of Periodontics & Restorative Dentistry (2021) concluded that socket preservation is cost-effective in virtually all cases where implant placement is planned.
Can I get dental implants if I’ve already lost significant bone?
Yes. Modern implant dentistry has solutions for even severely resorbed jaws. Options include bone grafting (guided bone regeneration, block grafts, sinus lifts), zygomatic implants that anchor into the cheekbone, short implants designed for reduced bone height, and All-on-4 protocols that use tilted implants to maximize existing bone. The key is comprehensive 3D imaging to map exactly what bone is available and developing a treatment plan that works with your specific anatomy. At Smile Dental Center, we handle complex bone-loss cases regularly and can outline all available options during your consultation.
Don’t Let Bone Loss Limit Your Options
Whether you’re planning an extraction, recently had one, or have been living with missing teeth for years, the sooner you get a 3D scan and consultation, the more options you’ll have — and the less it will cost. Our CBCT imaging shows exactly how much bone you have and what’s needed to achieve stable, long-lasting implants.
Message us on WhatsApp or call (786) 560-7567 to book your consultation.




